
A key factor in minimally invasive knee surgery is protecting and preserving muscles. This is particularly true for knee joint replacement or resurfacing. The muscles provide strength and control of your knee. The muscles are also an important factor in regaining motion. As you would expect, not cutting or detaching muscles around the knee results in less pain, better motion and faster recovery.
There are a number of different surgical approaches to the knee joint. The most common knee incision is the “peripatellar” incision (Fig. 1, Left). This incision has the advantage of being technically easy for the surgeon and provides good exposure to the knee. A disadvantage of this approach is that it detaches one third of the quadriceps muscle. The quadriceps muscle is the big muscle on the front of your thigh and attaches to the upper part of the kneecap. Although the incision in the muscle and tendon is repaired at the end of the procedure, patients with knee replacement through this approach tend to have more pain. Muscle activity of the leg pulls on the suture line in the muscle. Detachment of the muscle also results in weakness. Patients with peripatellar incisions are much less likely to be able to lift their leg the day (straight leg raise) after surgery.
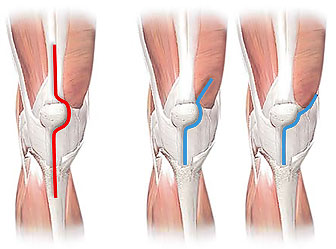
Fig. 1. Surgical approaches to the knee.
Left: peripatellar knee incision (red line); vastus medialis muscle (* ) is detached from quadriceps tendon;
Center: midvastus knee incision; vastus medialis muscle (* ) is partially split (short red line)
Right: subvastus knee incision; vastus medialis muscle (* ) is left intact.
An alternative approach is the “midvastus” approach (Fig. 1, Center). This is a slight improvement over the peripatellar approach; however, it still cuts into the muscle.
The subvastus approach (Fig. 1, Right) is a truly “quadriceps-sparing” surgical technique. The entire quadriceps muscle is left intact. As you would expect, patients who have a total or partial knee replacement with the subvastus approach have less pain, better muscle control and overall faster recovery.
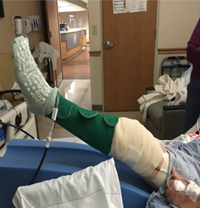
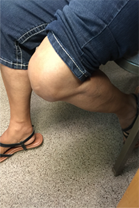

Fig. 2. Left: Patient able to do straight leg raise one day after subvastus quadriceps-‐ sparing total knee replacement. Center and Right: range of motion after subvastus total knee replacement.

Fig. 3. Dr. Grimes performed a subvastus approach knee replacement on Louise. Three months later, she was able to take her dog, Uno, through performance competition trials and won!
Some patients have arthritis that primarily involves only one compartment of the knee. The most common is the inside or ‘medial’ part of the knee. This can be treated with resurfacing of only the arthritis part of the knee (Fig. 4, Left). Performing this operation through a subvastus approach, as described above, makes the procedure less invasive. Some patients are able to go home the same day or spend only one night in the hospital.
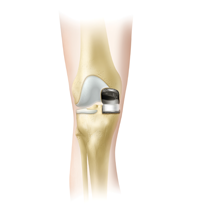
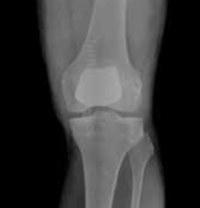
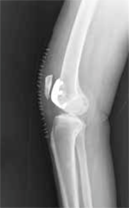
Fig. 4. Left: Unicompartmental knee resurfacing (“UNI”), which resurfaces only the inside (medial) part of the knee; Center and Right: Kneecap Resurfacing. This operation resurfaces the kneecap and the part of the thighbone where the knee cap slides .
Some patients have advanced knee arthritis that primarily involves the kneecap. If other treatments are ineffective, the kneecap and the part of the thigh bone where the kneecap slide (trochlea) can be resurfaced. This procedure can also be performed through the subvastus approach.
Knee procedures performed through the subvastus approach are more technically demanding than procedures performed through a conventional incision. Dr. Grimes has over 20 years experience performing subvastus minimally invasive knee procedures. Although not all knee procedures can be performed with this approach, it offers definite advantages over more traditional incisions. To learn more, call us for an appointment at 661-324-2491 in Bakersfield.
For more information click Success Stories tab below